by Hailey Branson-Potts, Alejandra Reyes-Velarde, Matt Stiles andAndrew J. Campa, LA Times
For Lupe Martinez, who does the laundry at a Riverside nursing home, each day presented an agonizing choice: Go to work and risk getting the novel coronavirus or lose the $13.58-an-hour paycheck her family relies upon.
Martinez went to work.
Even after the masks started running low. Even, she said, after a patient whose room she had entered without protective equipment fell ill and was put into isolation.
Martinez, 62, tested positive for COVID-19 last month, followed by her 60-year-old husband, who had to stop working after having a heart attack last year. Her adult son and daughter, who live with them, also tested positive.
“There were many times I didn’t want to go to work,” said Martinez, coughing heavily as she spoke. “I didn’t want to get sick. My husband said, ‘Don’t.’ I said we can’t live. We have these bills. … I had to push myself to go. I had a commitment to my family.”
For low-paid employees whose work is rarely if ever glorified — the people who clean the floors, do the laundry, serve fast food, pick the crops, work in the meat plants — having the jobs that keep America running has come with a heavy price. By the odd calculus wrought by the viral outbreak, they have been deemed “essential.” And that means being a target.

Along with blacks, Latinos have borne the brunt of the COVID-19 pandemic in California and other parts of the United States, becoming infected and dying at disproportionately high rates relative to their share of the population. Health experts say one of the main reasons Latinos are especially vulnerable to COVID-19 is because many work in low-paying jobs that require them to leave home and interact with the public.
Latinos comprise about 40% of California’s population but 53% of positive cases, according to state data. In San Francisco, Latinos comprise 15% of the population but make up 25% of the confirmed COVID-19 cases.
UC San Francisco researchers tested thousands of people in the city’s Mission District for COVID-19. While Latinos made up 44% of the people tested, they accounted for more than 95% of the positive cases. About 90% of those who tested positive said they were unable to work from home.
A Los Angeles Times data analysis last month also found that younger Latinos and blacks were dying at disproportionately high rates, belying the conventional wisdom that old age is the primary risk factor for death.
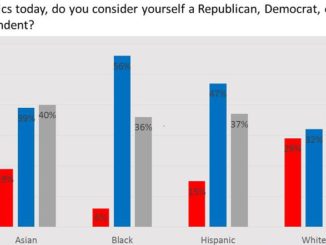
Latinos in California are significantly less likely than whites, Asians and blacks to say that working from home amid the pandemic is an option, according to a new poll of California voters from the UC Berkeley Institute of Governmental Studies.
Some 42% of Latinos polled said they could work from home, compared with 53% of blacks, 59% of Asians and 61% of whites. The poll also showed that Latinos were nearly three times more likely than whites to be concerned about their jobs placing them in close proximity to others. This was a particular problem in the first weeks of the pandemic, when masks and other protective gear were in shorter supply and many businesses were still trying to implement social distancing policies.
“They feel essential; they’re trying to do their part to get us out of this crisis,” said Jose Lopez, a Los Angeles-based spokesman for the Food Chain Workers Alliance. “Yet we can’t provide face masks. We can’t give them the space to give them six feet of separation between their co-workers.”
A Times analysis of U.S. Census Bureau data shows that Latinos make up just under 40% of the workforce across all industry sectors deemed essential by the California state government, consistent with their share of the statewide population. But in some sectors, they are greatly overrepresented.
In essential agriculture jobs, the workforce is more than 80% Latino. They also hold more than half of essential food jobs and nearly 60% of construction jobs deemed essential. At the same time, Latinos in the U.S. are more likely than the overall population to say they or someone in their household has experienced a pay cut or lost a job amid the pandemic, according to a Pew Research Center survey in April.
For weeks, Dr. Marlene Martín, an assistant clinical professor at UC San Francisco and a physician at Zuckerberg San Francisco General Hospital, has watched as Latino patients with COVID-19 have streamed into the emergency room. More than 80% of the hospitalized coronavirus patients at the facility were Latino as of last month.
They have been roofers, cooks, janitors, dishwashers and delivery drivers. Many were under 50. They lived in households where social distancing is difficult, sometimes with two or three other families. For Martín, a 36-year-old Latina, stepping into the intensive care unit sometimes feels like being confronted with an unsettling mirror.
“It was already full of people who look like me,” she said, “who share a common language and similar cultural backgrounds.”
“You see the extremes of what happens when someone can shelter in place or someone can’t. It’s not that people don’t want to stay home. It’s not that they’re not listening. It’s not that they’re not educated. It’s that they don’t have an option.”
The coronavirus’ heavy toll on Latinos raises questions about whether employers across the U.S. and the government are doing enough to protect these workers.
In Iowa, Latinos make up about 6% of the population but have accounted for a quarter of all positive cases, according to the state’s tally. In Washington state, Latinos represented 35% of all positive cases, even though they only make up 13% of the population.
The balance between keeping Latino essential workers safe and depending on their labor is being tested in the city of Hanford, where a coronavirus outbreak at a meat-packing plant now accounts for half of the confirmed cases in Kings County.
About 180 employees at Central Valley Meat Co. had tested positive as of Tuesday, according to County Supervisor Doug Verboon. Most of the employees at the facility — who work in close proximity amid “moist and wet working conditions” — are Latino, he said. Central Valley Meat did not respond to calls or emails from The Times.

Verboon said the county is depending on even more Latino workers during the current cherry-picking season, which lasts until mid-June. He said one Hanford fruit-packing company that employed 800 workers to pick cherries told him that an outbreak similar to the one at Central Valley Meat Co. would be “catastrophic.”
“We can’t have those people get ill because we have a short window of work,” Verboon said.
upe Martinez started at Alta Vista Healthcare & Wellness Centre in Riverside last July after her husband, a sheet metal worker and the family breadwinner, had a heart attack and had to stop working.
In the laundry room, Martinez — a member of the Service Employees International Union Local 2015, which represents some 400,000 home care and nursing home workers in California — was surrounded by mostly Latinos and Filipinos. A lot of her colleagues work two jobs or pull double shifts, washing heavy comforters and blankets, cleaning shower curtains, handling patients’ linens.
Martinez’s family asked her not to go as the virus began spreading in California.
“I told them, ‘I’m going to trust God. I’m not going to get it,’” she said. “I’d go to work. I’d worry.”
A few weeks ago, Martinez said, she walked into the room of an elderly woman to bring her clean clothes. Usually, there is a notice on the door if a patient has an illness that requires staff to put on gloves, masks or other gear, she said. There was nothing posted, Martinez said, so she entered unmasked.
Martinez said the woman told her she was feeling sick. A few days later, a sign on the door said she was in isolation.
Alta Vista Healthcare & Wellness Centre did not return calls or emails seeking comment.
On April 13, Martinez came home with a sore throat, dry cough and aching body. She couldn’t taste the tea her son brought her. She struggled to breathe. She went to the hospital before and after a positive COVID-19 test and was sent home, told to try and self-isolate.
When her husband, son and daughter who live in the house tested positive, she lay in bed, crying out to God.
Another son and his wife live in a back house on the property. He’s a barber. She’s a dental hygienist. They are not currently leaving home to work. They have not gotten COVID-19.
Because she had not yet worked at the nursing home a year, Martinez said, she was not eligible for sick pay. She has applied for state disability but has not yet heard back. Martinez said she feels she has to return to work.
“My kids don’t want me to go back,” Martinez said. “But I have bills. I know it’s my life, but — I don’t know.”
Rosa Arenas, another union member and certified nursing assistant at an Orange nursing home, said she got tested after learning a patient had tested positive for COVID-19 last month. On May 2, Arenas tested positive.
Now, she is isolated in one bedroom of her family’s apartment, away from her husband and two children, ages 12 and 6, who have tested negative. She spent Mother’s Day reading the Bible alone and video-chatting with her children and husband from the other side of the door.
“My kids told me they were sad they weren’t going to give me a Mother’s Day hug,” Arenas, 32, said. “It broke my heart.”
She said there was not enough personal protective equipment at work and that colleagues have become infected. Her husband, a landscaper, recently was sent home by his employer to quarantine and be tested, and she has burned through all her paid vacation and sick time while quarantining at home. And she misses working.

When Rafael Saavedra, a 40-year-old truck driver from Alhambra, returns home from work, he undresses in his garage, throws his clothes in the washing machine and rushes to the shower, careful not to touch anything inside. His greatest fear is infecting his daughters, ages 16 and 6.
At a San Pedro dispatch center, where he and hundreds of other drivers drop off paperwork and take breaks, he hardly ever finds soap or hand sanitizer.
Employees who normally work in the center are now working remotely, and there’s little communication with drivers about how they can stay safe, Saavedra said. Drivers were given a single, thin mask about a month ago and nothing else, he said.
Saavedra said the vast majority of drivers he works with are Latino immigrants who are struggling to navigate the pandemic because of language barriers and a lack of resources.
“They don’t know their rights. They’re scared of talking. They stay in their cocoon,” he said.
Saavedra has carved out a comfortable life for his family. He travels often with his wife and daughters, who attend private Christian schools. But his paycheck has been cut in half due to reduced hours. He fears losing his house.
His wife, a nurse at a Pasadena homeless shelter, cut down her own hours out of fear of catching the virus and infecting their daughters.
Sonia Hernandez, who raised four children as a single mother, has worked as a cook at a McDonald’s in Monterey Park for 18 years and makes just over $14 an hour, said her daughter, Jenniffer Barrera Hernandez.
In early April, Hernandez was hospitalized with COVID-19 and went into an induced coma for weeks.
“They told us she wasn’t going to make it through the day and we had to decide whether she wanted to go in peace or do chest compressions to try and get a pulse,” Barrera Hernandez said. “It was really hard to make that decision.”
Miraculously, Barrera Hernandez said, her mother woke up.
After her diagnosis, Hernandez’s co-workers walked off the job to demand safety supplies, including masks, gloves, soap and hand sanitizer. Barrera Hernandez said after she called McDonald’s to alert the company her mom had tested positive, she did not get a call back.
“That’s really sad, because my mom really liked that job. You provide for a company for so long, and at the end you’re just a number.”
Hernandez is recovering in her South L.A. home. She is extremely fatigued and unable to walk or even hold a phone for very long, her daughter said. She feels guilty she can’t go back to work yet.
David Tovar, McDonald’s U.S. vice president of communications, said many of Barrera Hernandez’s and some employees’ statements were false.
He said McDonald’s restaurants, including the one where Hernandez worked, have had an ample supply of soap, hand sanitizer and cleaning supplies and close overnight once per week for deep cleanings. Tovar said restaurants have been open for takeout only, with social distancing requirements enforced and bathrooms closed.
When McDonald’s learned of Hernandez’s diagnosis on April 8, the company immediately informed four crew members who she had been in contact with, he said.
“We have the utmost respect for Ms. Hernandez and all the employees at McDonald’s, but it’s unfair to let them try to tell a story to you that’s simply not true,” Tovar said. “We are a very large employer of diverse employees, particularly Latinos. We want everyone who comes to work for McDonald’s to have a good experience.”
When Mariana Lui’s mother got a letter from her employer in March that labeled her an essential worker, she announced it with a sense of pride.
Lui’s mother, an undocumented immigrant from Mexico who works at a San Fernando food production warehouse that makes meals for schools, told her daughter that she had never before been deemed “essential.” Now, she said, people needed her.
But then her colleagues, many of them undocumented Latinas, started getting sick. They stopped showing up on the assembly line, where, she said, they stack ingredients onto sandwiches while standing shoulder to shoulder.
Lui’s mother spoke to The Times on the condition of anonymity because she feared losing her job. Lui, who also spoke to The Times, is a 31-year-old legal administrative assistant in Whittier with a different surname than her mother.
Lui’s 50-year-old mother said colleagues were taking aspirin and continuing to work, despite having fevers and headaches. Then she started showing symptoms.
“I was getting tired at work and I had a little bit of a cough,” she said. “I didn’t think it would be something so serious, so I kept going to work for three or four days.”
A few days later, she tested positive for COVID-19.
Hailey Branson-Potts is a Metro reporter for the Los Angeles Times who joined the newspaper in 2011. She grew up in the small town of Perry, Okla., and graduated from the University of Oklahoma.